
30% of surveyed radiation oncologists said #priorauthorization has caused emergency room visits, hospitalization or permanent disability for their patients.
7% said it led or contributed to a patient’s death.
This data is clear.
We need to #fixPriorAuth
www.astro.org/news-and-pub...
06.12.2024 15:28 —
👍 57
🔁 26
💬 4
📌 2
laugh or cry? #pharmacy #priorauth #primarycare edition:
"Fax from the pharmacy for Duloxetine 40mg caps stating this is not covered. Per insurance, this drug requires a PA. Please consider switching to Duloxetine 20mg caps taking 2 a day."
11.04.2023 19:01 —
👍 3
🔁 2
💬 0
📌 0
Today I saw a patient who needs a PET scan to help us figure out how to most safely and effectively biopsy her cancer
PET scan appointment available Monday but was told it would be at least 2 weeks because of #priorauth
This is not how it is supposed to work
@MedicineForward
23.06.2022 20:01 —
👍 2
🔁 2
💬 0
📌 0
Just got a phone call from my primary care doc friend - their patient suddenly requires #priorauth for glargine.
INSULIN GLARGINE.
What in the actual bleeping bleep bleep.
Incidentally, patient has UHC.
Unacceptable.
#medsky #endocrinesky #primarycare
17.12.2024 22:07 —
👍 8
🔁 2
💬 0
📌 0
#medsky the latest turn of the screw in #priorauth is your peer refusing to identify themselves due to "safety concerns." Respecting their safety, ask 4 a supervisor. Or, ask for another identifier, like an employee ID. Get something. If they deny reasonable care, contact your congressperson 1/2
17.01.2025 16:39 —
👍 11
🔁 5
💬 2
📌 0
Real case: 32 week pregnant patient with raving bacterial vaginosis had her Flagyl denied. BV can cause preterm labor and serious complications. GoodRx cost of drug: less than $20.
08.02.2025 01:34 —
👍 2
🔁 0
💬 0
📌 0
Yup and what are the chances that it will still be denied and will require an hour long phone call from the provider? Nearing 100% I'm sure.
08.02.2025 01:30 —
👍 3
🔁 1
💬 0
📌 0
Sounds about right for those ghouls.
29.12.2024 01:08 —
👍 5
🔁 0
💬 0
📌 0

Inside the Company Helping America’s Biggest Health Insurers Deny Coverage for Treatments
When companies like Aetna or UnitedHealthcare want to rein in costs, they turn to EviCore, whose business model depends on turning down payments for care recommended by doctors for their patients.
Our seventh most-read story of this year: When companies like Aetna or UnitedHealthcare want to rein in costs, they turn to EviCore, whose business model depends on turning down payments for care recommended by doctors for their patients.
Read more (published October) ⬇️
29.12.2024 01:00 —
👍 3016
🔁 1608
💬 156
📌 204

Another patient had brillinta denied after MI. His cardiologist and I (PCP) fought with BCBS to the point where we sent cath lab notes and they said it was my fault because I answered not to a question that needed a yes. When I fixed it on the phone with a rep, they denied it again.
Brilinta (ticagrelor) is a medication that makes platelets less "sticky", ie stops clots. Used after someone has a stent placed in their coronary artery. NOT taking Brilinta can lead to a stent thrombosis: a blood clot inside the stent that was placed. Leading to another heart attack. Or death.
29.12.2024 01:06 —
👍 3
🔁 0
💬 0
📌 0

I now have to get a new prior authorization for Mounjaro for one of my diabetic patients every time I increase the dose. Her A1c is > 10. Every time I do the PA, it requires an appeal. For the same med they're already approved.
Even when we've made our case to them and they've approved, they still try again to not pay for appropriate care.
28.12.2024 18:19 —
👍 5
🔁 1
💬 0
📌 0
Why am I zero percent surprised it was United?
27.12.2024 16:34 —
👍 1
🔁 0
💬 0
📌 0
We need to be screaming these examples from the mountain tops to keep people in the public aware of the ghoulish behavior of the insurance industry.
21.12.2024 00:22 —
👍 7
🔁 0
💬 0
📌 0
This was denied
I did everything I was asked
This is a necessary generic med
The system is broken
I am broken
20.12.2024 22:51 —
👍 142
🔁 32
💬 27
📌 3

Comprehensive ophthalmology
72 year old man with glaucoma in both eyes. Already blind in his right eye from glaucoma. Now with worse vision in the left eye making him unable to drive. I planned for combined cataract surgery with glaucoma surgery in his left eye to prevent blindness in his ONLY seeing eye. We get prior authorization from UHC for both cataract surgery and glaucoma surgery.
I perform surgery, and he has incredible results. He can finally see well enough to drive himself and his eye pressure is significantly improved.
Get paid $490 for the cataract surgery but glaucoma surgery is denied (mind you we had a PA but of course “that’s not a guarantee of payment). I appeal x2 and finally get notified that we cannot appeal again and their decision is final. I cannot justify charging the patient for the surgery so I did it for free.
So even if we get a prior authorization you might not pay us? Cool and good.
19.12.2024 19:37 —
👍 8
🔁 2
💬 3
📌 1
I mean... I posted several accounts from verified physicians today. Insights: insurance companies want to make money and they do that by denying care.
19.12.2024 19:30 —
👍 2
🔁 0
💬 0
📌 0

I had a young 21 year old male, who had a traumatic patella dislocation and MCL injury. I was able to get a surgery spot in 6 days. The ligament (MPFL) that holds the patella in place was ruptured and insurance approved repair. But denied the MCL repair, even though it was 100% torn AND the torn end flipped under 180 degrees creating a 2cm gap. They said he had to do at least 6 weeks of physical therapy. This MCL has a 0% chance of healing EVER without a repair, and therapy won’t make one lick of difference. And you make someone wait 6 weeks for repair and it’s no longer repairable. At that point if anything it is a reconstruction (rebuilding) with cadaver tissue. Athlete or not I’d fix that EVERY TIME as standard of care. Give me a 60 year old in a desk job that likes to hike casually on the weekend or a 45 year old laborer and I’d still fix that 100% of the time. It is not only piss poor care for the patient, it’s a huge individual financial loss not to mention a societal loss to have someone out of work for potentially 6 months because insurance says I need to wait to treat the MCL the right way.
It’s criminal and unethical for the insurer to dictate care like this.
19.12.2024 19:27 —
👍 2
🔁 0
💬 0
📌 0

Adult psych in community mental health setting, which means severe mental illness in the outpatient setting. I had a patient with Bipolar 1 with psychotic features who had been hospitalized for mania and and psychosis at least 10 times. Multiple trials of mood stabilizers and every antipsychotic you can imagine. Only medicine he responded to was Clozaril. He has a history of anaphylaxis to one of the non-active ingredients in the generic, so he needed brand name. He had been on this medicine for 5 years, and for that entire time he was stable without any hospitalizations, psychosis, or mania. One January insurance company just suddenly decided to not approve it. We appealed. Appeal denied. We appealed again, long written letters. Denied. Peer to peer. Denied. I went back and forth with the insurance company for a whole month. The day he took his last pill I spent 5 hours on the phone with the insurance company. Never mind that I had a full schedule with other patients. This was potential for crisis. I *finally* got someone who explained that clozaril was full stop no longer covered for bipolar disorder with psychotic features. It was only covered for schizophrenia and schizoaffective disorder bipolar type. On the phone I said, "oh, well there's been a change in symptoms and he has now been diagnosed with schizoaffective disorder bipolar type." And the approval went through at that point. OMFG I have never been so furious.
19.12.2024 19:25 —
👍 1
🔁 0
💬 0
📌 0

Patient with large fibroid uterus and a chronic hemoglobin of 5. Insurance would not approve admission the night before to get her hemoglobin to a safe level to operate. Said she could have a separate admission for that, which she would have just bled off before the surgery. Peer to peer appeal review was futile so I asked, “do you have a medical degree, a medical license, and do you or have you ever practiced medicine?” The answer to all of those questions was “that is not relevant”. Like hell it is not. Next question I asked was “what would you want done if this were you, your sister, or your daughter.” Silence…and still not approved. I admitted her and proceeded with the plan anyway as it was the only right thing to do.
Explain to me how someone with no medical training gets to tell us how to practice medicine?
19.12.2024 19:22 —
👍 1
🔁 0
💬 0
📌 0
Adult ID: patient stable with undetectable HIV viral load who has been on a given med for YEARS. Suddenly needs PA that is denied despite peer review.
Patient with invasive fungal infection who needs Cresemba. Denied. You can use fluconazole (which doesn't work for anything other than candida).
19.12.2024 19:20 —
👍 1
🔁 0
💬 0
📌 0
A pediatrician shared that an MRI ordered on a child for neck pain showed a slight glimpse of a brain tumor at the base of the brain. Called by imaging center for order for MRI brain. Insurance company denied until a Peer to Peer and PA was done while the child was still in the MRI scanner.
19.12.2024 19:17 —
👍 1
🔁 0
💬 0
📌 0

- I spend a lot of time appealing medication denials for medications that patients have already been taking. I'll have kids on Humira who are doing great, been on it for x amount of time, and insurance will suddenly send a denial letter. I then have to drop everything I'm doing to get the medication reapproved so the child can get the next dose in time. These are random denials in addition to usually having to get the medication reapproved every January. I've had kids have to live off samples because their insurance companies are taking their sweet time despite urgent appeals. These are extra egregious for biologics because late doses put people at risk of developing antibodies that will render the medication ineffective
From a pediatric Gi physician. It's not just the adult lives they're willing to sacrifice.
19.12.2024 19:14 —
👍 1
🔁 0
💬 0
📌 0

Patient in her 60s with recurrent cervical dysplasia. Had previously had multiple excisional procedures such that her cervix was flush to the vaginal wall and no longer safe to continue to try to excise. Patient had persistent, mild dysplasia with inadequate colonoscopies due to the flush, cervix and stenosis. The only option left at that time was a hysterectomy, which was denied even with a peer review. during the peer review the physician that I was talking to refused to tell me what other options the insurance required before they would approve the hysterectomy. Flat out refused to tell me why it was being denied with the comment of “I’m not her doctor so I can’t tell you how to practice and take care of your patients” 😡
Apparently they won't tell us how to practice medicine. They just won't pay for what we suggest.
19.12.2024 19:10 —
👍 1
🔁 0
💬 0
📌 0

DrByronHapner
@DrByronHapner
Follow
Hey @UHC. Completed a hysterectomy yesterday afternoon, discharged her home in the evening (saving @UHC and everyone some money). Discharge medications included 12 Vicodin. (retail cost $30). Vicodin DENIED pending prior authorization. Patient in pain all night. Way to go.
12:16 PM • 12/10/24 • 4.2M Views
Not even the death of their CEO can make them change their ways
12.12.2024 17:46 —
👍 203
🔁 59
💬 13
📌 4
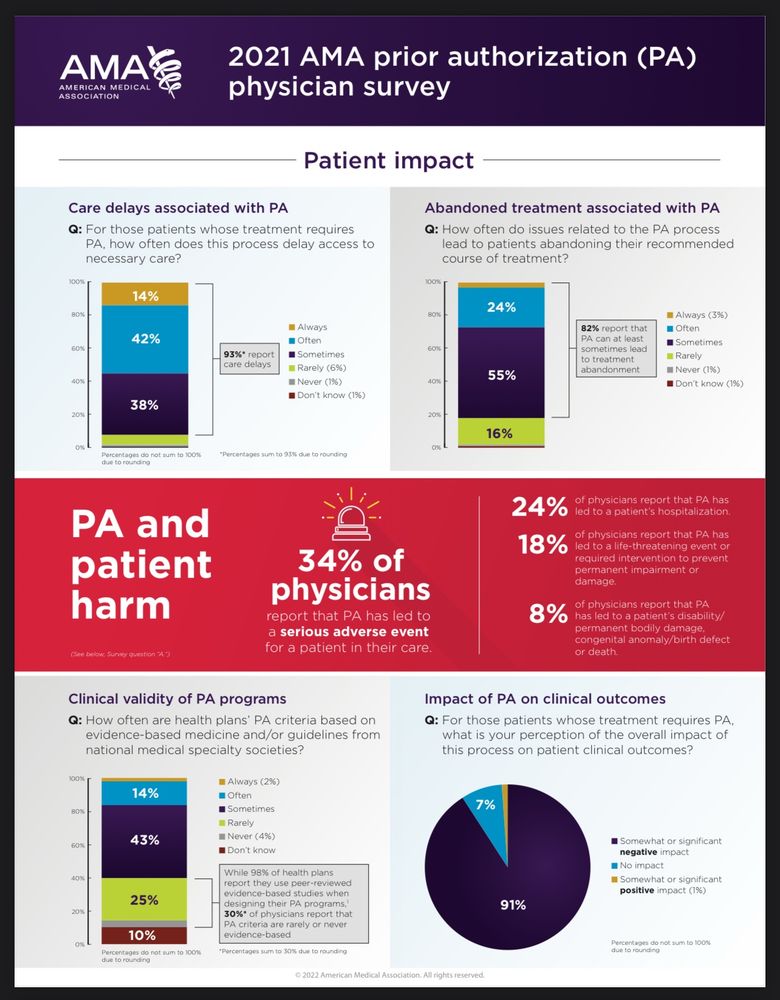
Infographic summarizing negative outcomes documented from prior authorization

Infographic summarizing negative outcomes documented from prior authorization
The American Medical Association surveyed doctors about insurance “prior authorizations” and found:
41 prior auths per doctor per week
13 hours spent per week on prior auths
24% reported hospitalizations due to delays from prior auths
8% reported disability/deaths due to delays from prior auths
12.12.2024 23:25 —
👍 905
🔁 437
💬 33
📌 39












