
7/ 📖 Monogenic disorders of immunity: Common variants are not so rare
Cell Genomics (2025)
🔗 www.cell.com/cell-genomic...
#Immunology #HumanGenetics #InbornErrorsOfImmunity #IEI #Genomics #PopulationGenetics #PrecisionMedicine

7/ 📖 Monogenic disorders of immunity: Common variants are not so rare
Cell Genomics (2025)
🔗 www.cell.com/cell-genomic...
#Immunology #HumanGenetics #InbornErrorsOfImmunity #IEI #Genomics #PopulationGenetics #PrecisionMedicine
6/ This argues for stronger dialogue in clinical immunology (and other medical fields) between patient-based and population-based genetics —biology and medicine sit at their intersection.
09.01.2026 15:13 — 👍 1 🔁 0 💬 1 📌 0
5/ Practical consequences in the field of clinical immunology at large:
🔹 For clinical genetics: stop using frequency as an exclusion criterion.
🔹 For population genetics: common variants deserve mechanistic and clinical follow-up —in “monogenic” frameworks they can have large effect.

4/ We compile and discuss examples of common variants across 14 immunity genes, illustrating how they can cause or shape monogenic disorders with high or low penetrance.
09.01.2026 15:13 — 👍 1 🔁 0 💬 1 📌 03/ Pathogenicity should be evaluated through functional impact, penetrance, and context, not MAF thresholds alone.
09.01.2026 15:13 — 👍 0 🔁 0 💬 1 📌 0
2/ “Monogenic” ≠ “rare.”
Allele frequency is a population metric — not a proxy for biological or medical impact.

🧬 New in @cellpress.bsky.social 🧵
1/ With @casanovalab.bsky.social , we propose a rethinking of monogenic disorders of immunity:
👉 common variants can matter — a lot.
Thank you to all the fantastic collaborators involved in this story. @casanovalab.bsky.social, and all not on bluesky, in particular Marie Materna, Simin Seyedpour, Tom Le Voyer, Nima Parvaneh, Niloufar Yazdanpanah, Jacinta Bustamante, Mohammad Shahrooei and Nima Rezaie
06.06.2025 11:10 — 👍 2 🔁 0 💬 0 📌 0Please consider submitting your work to @jhumimmunity.org, the novel journal of the “Inborn Error of Immunity” community. It is published by the nonprofit @rupress.org
06.06.2025 11:10 — 👍 4 🔁 3 💬 1 📌 0
🧩 Conclusion:
The absence of ⍺β T cells is sufficient to cause SCID. γδ T cells and other leukocytes cannot compensate for this loss.
🧬 Our molecular data show:
• New variants = complete loss-of-function → total absence of ⍺β T cells
• Original c.+1G>A variant = partial loss-of-function → low TCR⍺β expression & unconventional ⍺β T cells, explaining longer survival without transplant
In our study, we report 2 patients from unrelated families with novel TCR⍺ variants. Unlike earlier cases, they presented with severe combined immunodeficiency and early, life-threatening infections.
06.06.2025 11:10 — 👍 2 🔁 0 💬 1 📌 0This suggested that lacking ⍺β T cells results “only” in combined immunodeficiency (CID), not severe combined immunodeficiency (SCID)—likely due to compensation by γδ T cells.
06.06.2025 11:10 — 👍 2 🔁 0 💬 1 📌 0
Previously, TCR⍺ deficiency was reported in 5 patients from 3 kindreds, all carrying the same variant (c.+1G>A). Despite the absence of conventional ⍺β T cells, these patients survived into childhood without early transplant.
📖 www.jci.org/articles/vie...
🚨 Our first paper in @jhumimmunity.org just came out!
We describe two forms of TCR⍺ deficiency: a complete and a partial form.
👉 doi.org/10.70962/jhi...
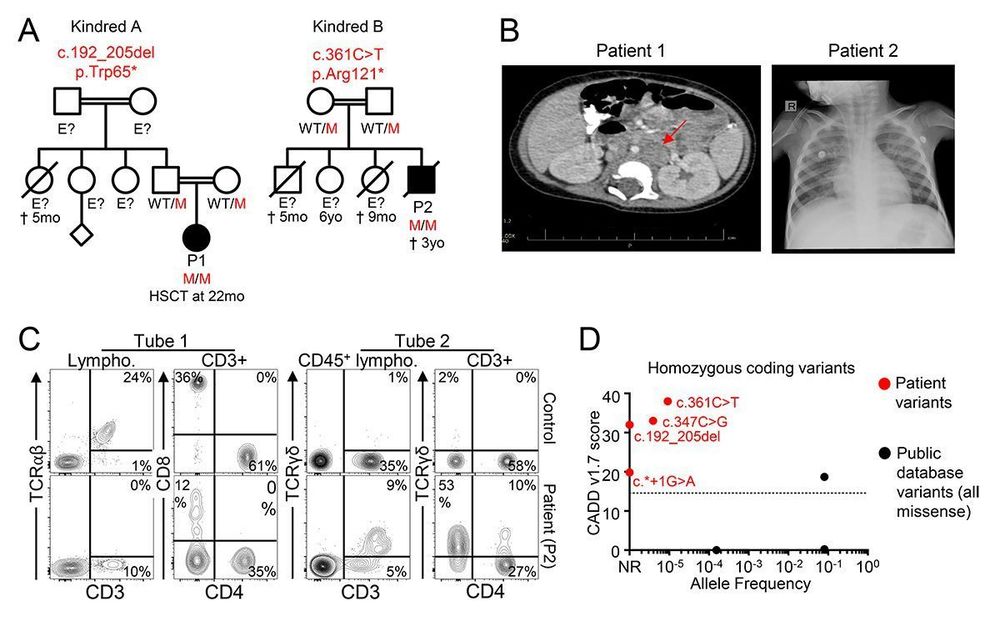
Materna, @vbeziat.bsky.social et al. @institutimagine.bsky.social report children with complete TCRα deficiency, a lack of αβ T cells, & a severe condition. Previously characterized TCRα deficiency, which wasn't as severe as expected, was partial, as opposed to complete rupress.org/jhi/article/...
04.06.2025 20:07 — 👍 5 🔁 3 💬 0 📌 0
New in @jhumimmunity.org: Materna, @vbeziat.bsky.social et al. report children with complete TCRα deficiency, a lack of αβ T cells, & a severe condition. Previously characterized TCRα deficiency, which wasn't as severe as expected, was partial, as opposed to complete rupress.org/jhi/article/...
04.06.2025 20:24 — 👍 3 🔁 1 💬 0 📌 0