
Open call for papers, Emerging Challenges in Long-Term Care and Caregiving. Conference to be held in Cambridge, MA on October 2, 2026. Submit papers by 11:59pm EDT on July 31, 2026. More information: www.nber.org/calls-papers...
24.02.2026 23:18 —
👍 2
🔁 1
💬 0
📌 0

Mentoring Program on Aging and Health Economics Research
Are you a PhD Student curious about working in topics of health and aging? Do you feel like you may need extra support? I have a program for you!
A one-day mentoring workshop hosted by yours truly and Jetson Leder-Luis (BU) through @nber.org
www.nber.org/calls-papers...
23.02.2026 16:12 —
👍 12
🔁 7
💬 0
📌 2

Opinion | The Trouble With MedPAC
A federal advisory board tries to undermine Medicare Advantage.
Sure, WSJ. Shame on me for worrying about patient access to care and taxpayer spending over for profit companies. As long as the system works for the wealthy it must be fine with you. Enjoying the comments on the piece, though.
Trouble With MedPAC - WSJ share.google/M9VyVAt9V255...
11.02.2026 00:56 —
👍 43
🔁 6
💬 6
📌 3

More immigration into the US raises the number of health care workers and saves the lives of older Americans, from David C. Grabowski, Jonathan Gruber, and Brian E. McGarry www.nber.org/papers/w34791
10.02.2026 14:02 —
👍 26
🔁 7
💬 0
📌 7

“We measure the impact of increased immigration on mortality among elderly Americans, who rely on the immigrant-intensive [health care] sectors… [we find] striking effects on mortality: a 25% increase in the steady state flow of immigrants to the US would result in 5,000 fewer deaths nationwide.”
09.02.2026 11:34 —
👍 29
🔁 19
💬 1
📌 2

Is Immigration Good for Health? The Effect of Immigration on Older Adult Mortality in the United States
David C. Grabowski, Jonathan Gruber, Brian E. McGarry #34791
Abstract:
We measure the impact of increased immigration on mortality among elderly Americans, who rely on the immigrant-intensive health and long-term care sectors. Using a shift-share approach we find a strong impact of immigration on the size of the immigrant care workforce: admitting 1,000 new immigrants would lead to 142 new foreign healthcare workers, without evidence of crowd out of native health care workers. We also find striking effects on mortality: a 25% increase in the steady state flow of immigrants to the US would result in 5,000 fewer deaths nationwide. We identify reduced use of nursing homes as a key mechanism driving this result
Immigrants save Americans' lives: "...a 25% increase in the steady state flow of immigrants to the US would result in 5,000 fewer deaths nationwide. We identify reduced use of nursing homes as a key mechanism driving this result."
www.nber.org/papers/w34791
09.02.2026 12:42 —
👍 75
🔁 26
💬 1
📌 1

Major news outlets: Please consider prominently reporting what this all-star team of researchers has found.
www.nber.org/papers/w34791
09.02.2026 12:22 —
👍 102
🔁 60
💬 2
📌 7


SNF capacity is the bottleneck that keeps people waiting in ER hallways and make-shift hospital rooms. SNF beds are crucial to our health system. Since 2020, capacity is down 5%, with less slack, due to staffing shortages.
@jamainternalmed.com @mlbarnett.bsky.social: jamanetwork.com/journals/jam...
14.01.2026 03:49 —
👍 6
🔁 3
💬 0
📌 0

Trends in Skilled Nursing Facility Capacity from 2018-2025. It shows Certified beds, Estimated operating capacity and Actual census in millions. Certified beds are high. Estimated operating capacity & Actual census dropped in 2021 but rise in subsequent years.
Skilled nursing facility operating capacity in the US declined by 5% since 2019, with the largest losses in rural counties and areas reporting staff shortages, impacting hospital discharge and access to facility-based postacute care. ja.ma/49LZK1E
12.01.2026 16:30 —
👍 0
🔁 1
💬 0
📌 0
More on dementia & finances: similar to credit outcomes, we see declines on asset side start about 6 years before dementia onset, patterns are consistent with mistakes driving declines, not healthcare spending or spenddown
13.01.2026 19:05 —
👍 15
🔁 5
💬 0
📌 0

Shortage at nursing homes have left an increasing number of patients in hospitals
Complex patients who need long-term care are struggling to find care in skilled nursing facilities. Researchers say staffing shortages play a huge role.
Our findings are very much consistent with media reports of hospital bottlenecks due to a lack of available SNF beds and underscore the importance of adequate SNF capacity for the flow of patients through the health care system www.npr.org/2024/05/13/1...
13.01.2026 13:51 —
👍 0
🔁 0
💬 0
📌 0
In summary, SNF operating capacity declined substantially during pandemic, likely due to staffing shortages, with a slow and incomplete recovery through 2024. Declines raise concerns about patient access to SNF care, esp. in rural areas, and ability of hospitals to d/c patients in a timely manner.
13.01.2026 13:51 —
👍 0
🔁 0
💬 1
📌 0

Finally, we find suggestive evidences that declines in SNF capacity have had upstream effects on hospital discharges. Hospitals where nearby SNFs had larger capacity declines have seen larger increases in length of stay and increases in the distance patients need to travel to an admitting SNF.
13.01.2026 13:51 —
👍 0
🔁 0
💬 1
📌 0

We found evidence that changes in SNF capacity were highly correlated with how frequently facilities reported staffing shortages, consistent with reports that an inability to hire and retain staff was forcing facilities to take beds offline or close entire SNF units.
13.01.2026 13:51 —
👍 0
🔁 0
💬 1
📌 0

We also found substantial geographic variation in post-pandemic changes in SNF operating capacity. 1/4 of counties experienced capacity declines of >15% 2024 vs. 2019. The counties with the largest declines were more likely to be rural.
13.01.2026 13:51 —
👍 0
🔁 0
💬 1
📌 0

Time series graph showing changes in licensed SNF bed counts, estimated operating capacity, and actual SNF patient census 2018-2024. Declines in operating capacity were greater than declines in licensed SNF beds
We studied this issue through 2024, finding only modest declines in the # of licensed SNF beds. But when we infer actual operating capacity (using max census over last 60 days), we find much larger declines. Operating capacity was down ~15% in 2021Q1 & remained 5% in 2024Q4 vs. 2019.
13.01.2026 13:51 —
👍 0
🔁 0
💬 1
📌 0

More than 400 nursing home closures projected for 2022: report
There have been more than 300 nursing home closures during the pandemic and another 400 could go out of business this year.
SNFs were hit hard during pandemic (>200,000 resident deaths, staffing shortages, declining patient referrals, rising operating costs). These headwinds raised concerns that many SNFs would be forced to close www.mcknights.com/news/more-th...
13.01.2026 13:51 —
👍 0
🔁 0
💬 1
📌 0

Nursing home effort fluctuates with the inspection cycle, affecting patient survival. Unpredictable inspection schedules may boost effort and save lives, from Ashvin Gandhi, Andrew Olenski, and Maggie Shi www.nber.org/papers/w34491
15.12.2025 17:00 —
👍 7
🔁 7
💬 0
📌 0

Asset Spend-Down and Medicaid Enrollment in Nursing Homes
This cohort study examines the rate of Medicaid spend-down among nursing home residents enrolled in traditional Medicare and assesses what factors are associated with Medicaid spend-down among these r...
Medicaid “spend down” — how we force individuals to impoverish themselves to qualify for Medicaid coverage of long-term care — is one of the most messed up things I’ve learned about the US health care system
In a new paper, we look at how often spend-down happens in nursing homes specifically
08.12.2025 14:10 —
👍 40
🔁 15
💬 3
📌 3

Next up at @SHESG2025, Katherine Wen presents work on employment and vaccine mandates. Katherine and her colleagues study the impact of vaccinations mandates surrounding COVID. You may remember that there was significant push-back from workers about the mandates at the time.
20.09.2025 13:56 —
👍 2
🔁 1
💬 1
📌 0
Excited this paper is out. Medicare Advantage is driving longer hospital lengths of stay, especially for patients discharged to SNFs. This has important implications for patients' access to post-acute care and hospital patient flows as MA becomes dominant type of Medicare coverage
09.09.2025 17:20 —
👍 5
🔁 0
💬 0
📌 0
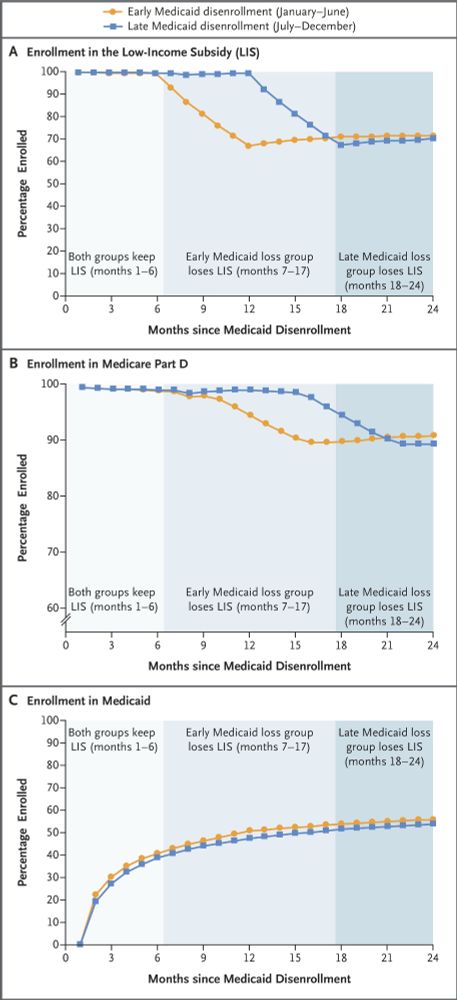
Loss of Subsidized Drug Coverage and Mortality among Medicare Beneficiaries | NEJM
A total of 14 million Medicare beneficiaries receive the Low-Income Subsidy (LIS),
which reduces cost sharing in Medicare Part D. Losing the LIS may impede medication
access and affect mortality. U...
Eric Roberts and @joefigs.bsky.social led a groundbreaking new study on Medicaid and Medicare, out today in NEJM. I’m lucky to have been a part of it.
Medicare saves lives. But is it enough to save lives of the most vulnerable Americans? The study suggests no; Medicaid still matters. (1/11)
14.05.2025 21:31 —
👍 73
🔁 38
💬 3
📌 8

Placing a "soft" spending limit on physical therapy reduces unnecessary care, but also introduces inequities based on how well providers can navigate paperwork requirements, from Ashvin Gandhi and Maggie Shi https://www.nber.org/papers/w33722
01.05.2025 17:00 —
👍 1
🔁 1
💬 0
📌 0
We are hiring! HSR, health policy, health Econ
jobs.academyhealth.org/jobs/view/as...
Happy to chat!
#econsky #policysky
06.03.2025 01:51 —
👍 11
🔁 10
💬 0
📌 2
A key problem is there's a Hotel California aspect to MA: once you're in, it's hard to leave.
In nearly every state, after your initial eligibility period @65, you can't revert to traditional Medicare without facing medical underwriting for Medigap plan that cover your out-of-pocket obligations.
08.01.2025 16:31 —
👍 9
🔁 6
💬 1
📌 1
As the baby boom generation enters its prime years for long-term care needs, its difficult to come up with a more challenging backdrop than an immigration system about to be cut off at its knees (think: nursing home aides) and states having to fill in funding gaps from Medicaid spending shortfalls.
25.11.2024 19:33 —
👍 159
🔁 71
💬 9
📌 4





















